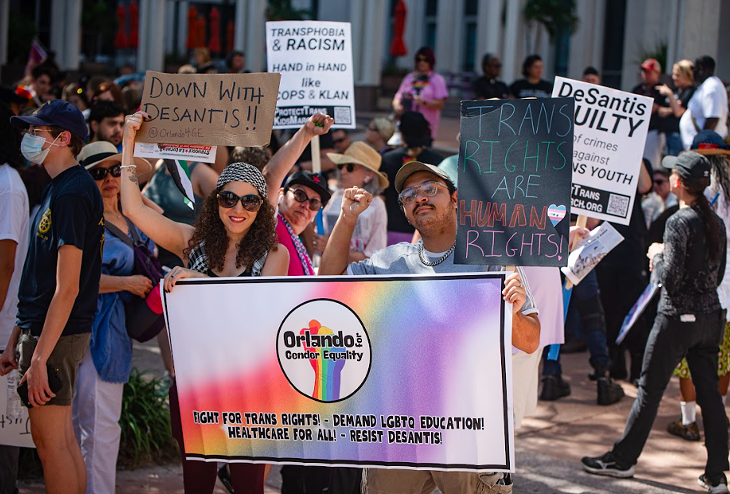Today, as executive director of the Orlando-based nonprofit Peer Support Space, she has what you might call “lived experience” with gaping holes in the mental health care system that exist not just in Florida but all across the country.
“I think we constantly tell people, you know, it's OK to get help,” Flasterstein, who uses she/they pronouns, told Orlando Weekly. “But like, we don’t spend enough time, I think, acknowledging that that help isn't always accessible, or it isn't accessible right away.”
Her experience has also inspired empathy with others who struggle to access to quality mental health care due to barriers like cost or availability. Too often, they can’t find a treatment provider who’s able to meet their needs.
This was a glaring problem in the aftermath of the 2016 Pulse nightclub shooting in Orlando, said Flasterstein, who was part of the emergency response to the tragedy.
The shooting left 49 people dead and dozens more wounded and traumatized. Many of the victims and survivors of the massacre were LGBTQ+, Latinos and people of color. It was Latin Night at the club when a shooter opened fire early in the morning at 2 a.m.
After the shooting, Flasterstein said, “It was really hard to find mental health providers for people that had intersecting marginalized identities.” There was a shortage of Latino treatment providers, culturally competent professionals who could help them heal from their trauma.
“Nobody understands the nuances of a community quite like a community itself,” said Flasterstein.
That’s why they’ve worked to harness the power of that kind of community support in the years since through Peer Support Space, a grassroots organization first established in 2019.
And today, they’re looking to take on their biggest project yet: After the nonprofit was forced to close a drop-in center they opened just ahead of the pandemic, they're now looking to open a mental health peer respite center for adults 18 and older to help fill a care gap in Florida, as similar facilities have elsewhere.
It’d be the only one of its kind in Central Florida, and the only one still in operation in Florida, after a respite center in Gainesville closed its doors several years ago.
According to Flasterstein, it's been years in the making. “When I started Peer Support Space almost five years ago, it was because I wanted a peer respite,” Flasterstein shared, her excitement bubbling over on the phone. “So this has really been a long time coming and it's coming to fruition now.”

Peer respite centers: ‘A break from hardship’
Peer respite centers, sometimes referred to as hospital diversion programs, are voluntary, short-term programs that offer community-based, nonclinical support, generally for mental health purposes.
They offer a comfortable, home-like environment for people who are struggling with mental health, but not experiencing an emergency requiring 24/7 supervision or medical attention.
A respite, different from a clinical inpatient setting, is “a break from hardship,” Flasterstein explains. What a peer respite allows you to do, she says, is to have an alternative to hospitalization. “‘I’m not in crisis, I just need to get away for a few days.’ I think that’s something we can all relate to.”
Peer respite centers have been around in some form for at least a couple of decades, although they're few and far between. As of 2018, there were less than three dozen across the country in total, with most of them concentrated in New York, California and Georgia.
Unlike medical settings, peer respite centers are run by people who have lived experience of behavioral health issues or navigating the behavioral health system. That is, people who intimately understand the challenges of the treatment landscape, and who can offer support from an informed place without judgment.
But it’s not just “sick people helping sick people,” as Flasterstein put it, referring to a common, but unfounded criticism of peer support services for mental health.The upcoming center in Orlando, planned to soft-launch in January and officially open to the public in February, won’t have medical professionals, but it will be staffed with state-certified peer recovery specialists.
No medical doctor, no psychiatrist. Prescription medication will not be administered on the premises, but people are welcome to bring their medication to safely store in their rooms.
It’s low-intensity, but therapeutic in its own right.
People don't always want to be “fixed” or analyzed or diagnosed, said Flasterstein. “Sometimes we want to stare at a wall for three days,” she joked (well, sort of). “Sometimes we want to just play video games, and do arts and crafts. Like, we just kind of need a physical space to get away from our home environment for a few days.”
Peer Support Space offers support groups, workshops, casual crafting get-togethers and a book club. While open to all adults over the age of 18, they’re focused on reaching historically underserved communities when it comes to behavioral health, such as immigrants, people of color, and adults in the LGBTQ+ community.
“[Peer support] is so not this thing that’s meant to replace traditional services, but to complement them and even get more people to use them.”
tweet this
Getting support from people with lived experience of behavioral health issues and from diverse backgrounds can be appealing to people who’ve found traditional treatments unhelpful, ineffective or lacking.
Everything at their peer respite will be voluntary. There’s no coercion. No forced treatment, which can for some be lifesaving during periods of crisis, but ineffective and traumatizing for others.
Even so, Flasterstein emphasizes that her organization doesn’t consider itself at odds with traditional treatments, nor do they want people to think what they’re offering can be a replacement for it.
“Research shows that when people use peer support, in addition to other traditional mental health services, their overall mental health isn’t just improved, but they’re actually happier with their therapists,” she shared. “So it’s very much so not this thing that’s meant to replace traditional services, but I think really complement them and even get more people to use them.”
There’s something uniquely comforting and therapeutic about talking to someone, connecting with someone who’s been where you are, emotionally or physically.
Last year, Florida lawmakers passed a law to promote peer support services by expanding training opportunities to become a certified peer recovery specialist.
An advisory from the federal Substance Abuse and Mental Health Services Administration shares that peer support workers can help demonstrate that recovery is possible, and foster a healing experience that is trauma-informed and focused on uplifting strengths, not weaknesses.
The need for support, be it professional, peer-run or a combination of both, is greater than ever. The COVID-19 pandemic exacerbated struggles with depression, anxiety, substance use and thoughts of suicide, particularly early on, as people lost their jobs, lost their loved ones, and found themselves more isolated, cut off from friends, family and their communities.
Suicide deaths, which increased over the last two years after declining from 2018 to 2020, are increasing fastest among people of color, young people and residents of rural areas, according to CDC data.
Marginalization based on one’s LGBTQ identity — discrimination, harassment — can also affect mental health. And policies trampling on the rights of LGBTQ community don’t help.
“I think it’s no secret that it's a hard time for LGBTQ+ people in the state of Florida,” said Flasterstein, who’s actively participated in and helped organize events in support of LGBTQ rights and immigrant rights. “A lot of times we are that kind of safe space, or we strive to be that safe space for that community.”

An overwhelming majority of Americans believe there is a mental health crisis in the country today. Yet there’s also a shortage of available treatment providers, which can leave overburdened hospitals and even law enforcement agencies left to pick up the slack, resulting in the criminalization of distress, or a revolving-door system, rather than lasting support.
Florida legislators have filed legislation for consideration in 2024 that aims to address a shortage of mental health providers in the state, noting in a news release that Florida ranks 43rd in the nation for its mental health worker-to-patient ratio and 46th in access to care, according to a report from Mental Health America.
Nearly 3 million adult Floridians have a mental illness, according to that report, but more than half did not receive treatment in the past year.
Over half of Americans with mental or behavioral health issues don’t look for care, or may be unable to access it because of financial or other logistical barriers. The wait list is too long, or maybe you lost your health insurance with your last job, or never had any in the first place.
Maybe you're able to get acute care, for crisis stabilization, but can't find an outpatient provider to work with after you leave a hospital — landing you back in the same environment and circumstances you left.
There’s limited research into peer respite spaces. But a representative of the federal Substance Abuse and Mental Health Services Administration recently told KFF Health News that they have proven themselves to be an “evidence-based model of care.”
There’s evidence to suggest they can reduce hospitalizations, and increase feelings of self-reliance and belonging. Peer specialists can also help people come up with proactive plans to respond to relapse or other crisis situations, should they arise in the future.
“When I’m in crisis, I don't know what I need,” Flasterstein explained. “But when I'm well, I know what I need.” Flastersein calls this a Wellness Recovery Action Plan.
What this can do is offer an actionable plan for when or if someone does find themselves in a crisis, which they can also give to loved ones. The plan can include information like reliable coping tools, a preferred hospital, and contact information for treatment providers to reach out to, if necessary. It could even include a rundown of what’s helpful to say and do — and what isn’t.
Peer Support Space also plans to offer holistic wellness options. “There’s kind of this limited view that mental health care equals therapy and medication,” said Flasterstein.Those treatments can be helpful, she says — even lifesaving — but it doesn’t always offer a complete picture. Caring for your mental health can also involve connecting with your spirituality, meditating, gardening, and simple things like doing arts and crafts, or getting some rest.
“Something that we hope people experience with staying at the respite is having an opportunity to expand their wellness tools, whatever that looks like for them.”
Getting ready for launch
The Orlando peer respite center will, admittedly, be a small operation. It will have three bedrooms, and allow for stays up to eight days. You must have a place of residence, outside of the respite. It's not intended to be a homelessness resource.
Critically, Flasterstein confirmed it will be entirely cost-free, thanks to funding they’ve received.
The Orange County Board of Commissioners this week approved $427,451 in funds received through the federal American Rescue Plan Act to support the project, although Flasterstein says their organization's primary source of funding is the Central Florida Cares health system.
They also have corporate sponsorships and individual donors, and they host fundraisers in order to diversify their funding sources, so they can continue to serve the community at no cost.
Two local Democratic legislators, State Rep. Anna Eskamani and State Sen. Linda Stewart, attempted to get $125,300 in state funds for the respite center through appropriations requests earlier this year.
Neither made it into the final budget, although it's uncertain that they would have been approved by Florida Gov. Ron DeSantis (who gets the final say), even if they had.
DeSantis, who has championed several anti-LGBTQ policies in the state, has in the past vetoed state funds requested for Orlando's Zebra Coalition, which serves LGBTQ+ youth, and for the LGBT+ Center of Orlando.
Eskamani, for her part, is glad to see that Peer Support Space has secured the funds they need to move forward with their project. In an email, she shared, “Peer Support Space is transforming the mental health space in Central Florida and is serving as a role model for other regions too.”
“I am excited to see this respite center open, and know it will save lives,” she added. An emailed request for comment from Sen. Stewart's office did not receive a response ahead of publication.
Orange County also funds a crisis intervention program for young adults up to age 24, run by Deveraux Advanced Behavioral Health. Young adults, and their loved ones, can access those mobile crisis services by calling 2-1-1.
Similarly, a behavioral health unit within the Orange County Sheriff's Office, in collaboration with Deveraux, also offers mobile behavioral health crisis services for adults or loved ones who call with nonviolent, mental-health-related emergencies.
The new peer respite will be located in the SoDo district, not far from the former Pulse site. Flasterstein said they plan to call their respite “Eva’s Casita,” in honor Eva Fajardo, a LGBTQ advocate and founding board president of Peer Support Space who passed away a year ago.
“She really believed that a missing part of our wellness was the ability to connect both with the earth and with one another.”
Subscribe to Orlando Weekly newsletters.Follow us: Apple News | Google News | NewsBreak | Reddit | Instagram | Facebook | Twitter | or sign up for our RSS Feed